Paul K is a sprightly young 72 year old who enjoyed tennis, walking and the outdoor life. About 12/52 ago he started to feel pain in both his legs and electric shocks going down the back of both legs. Gradually he was unable to continue with outdoor activities and spoke to his general practitioner about his problems.
The GP thought he had some neurological problems based on the symptoms that he was describing and referred him for radiological examination and consultation with an orthopaedic specialist.
This is a summary of the MRI report 05 March 2024
- normal appearances of the visualised distal cord down to the conus at the L-1 level. Degenerative changes in the marrow signal.
- Mild degenerative changes down to L2/L3
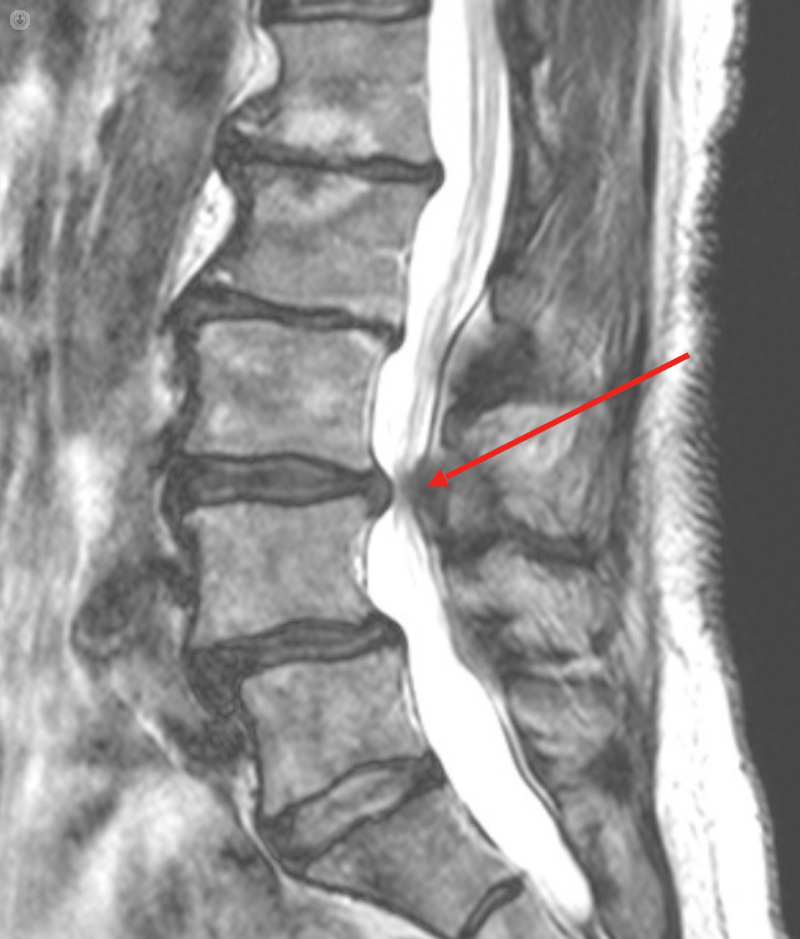
- L3/L4 – there is an extruded disc which causes moderate to severe central canal with almost complete effacement of the CSF within the thecal sac at this level. Mild bilateral neural foraminal stenosis.
- L4/L5 – minor degenerative disc bulge pressures the right L5 nerve in the right lateral recess and contacts the left L5 nerve. There is also severe right neural foraminal stenosis with potential right L4 neural compromise.
- L5/S1 – minor degenerative disc bulge which contacts the L5 nerves in the far lateral position bilaterally.
Conclusion:
-
There is moderate to severe central canal stenosis at the L3/L4 level.
-
The patient’s bilateral posterio-lateral leg pain could be caused by the potential bilateral L5 compromise.
Paul telephoned me from the UK concerned about his symptoms and his diagnosis from the radiologist. He asked my advice on whether I was able to help him instead of having surgery as the orthopaedist suggested.
He reported that there was no intermittent claudication associated with spinal stenosis, that both his legs felt strong and that he only experienced an electric shock in his legs and feet when he ran or was going downstairs. He experienced low back pain when standing for long periods.
I suggested that the symptoms did not match the radiologist comments and maybe the MRI pathology was incidental to his current symptom profile. He decided to fly to Portugal for a consultation and physical examination.
On examination I found he had pelvic instability, a physiological short-leg, a functional scoliosis of the lower spine, trigger points in the left sacroiliac ligament and muscle spasm running from the left sacroiliac joint up to the left occipito-atlantal joint just below the skull.
Treatment involved prolotherapy injection to the left sacro-iliac ligament. After three minutes the low back pain had disappeared, the spinal muscle spasm had gone and the legs were level. Three days later I did osteopathic manipulation to restore functional integrity of the spine. When he left, after seven days, he reported all his symptoms had disappeared apart from a mild low back pain which has been with him for many years.
In conclusion:
If Paul had followed the orthopaedist’s advice and had surgery for the spinal stenosis and the disc protrusions it might have been considered “failed back surgery” because the operation would have treated the results and not the cause.
It is important for patients to seek advice from a practitioner working and practising a different medical paradigm before consenting to surgical mutilation and statistical profiling.
We, at the Centre for Bioregulatory Medicine, considers everyone is an individual and decides the most appropriate treatment according to the patient’s needs. Surgery is sometimes the only solution if the pathology is severe but unnecessary surgery is a crime.
Criminal law does have a role to play when surgeons abuse trust and harm patients, but understanding when non-fatal surgical harm should be treated as a criminal matter is a complex issue.


0 Comments